What Causes Foot Stress Fractures?
While the occasional injury is part of an active lifestyle, some are more frustrating than others and some, caught early enough, can be avoided altogether. Stress fractures are in that category. Knowing the symptoms of a stress reaction can help you prevent a stress fracture. But, if you've already got a stress fracture, here's what you should know.
The Basics ---
- Weight-bearing exercises like running and walking are good for your bones as they promote the development of new bone cells. However, when your bones experience a repetitive application of force that is more than they can bear, a stress reaction or stress fracture can result.
- Stress fractures can occur in the feet, lower legs and upper legs.
- Athletes who engage in activities like basketball, tennis, gymnastics, track and field, and running have a higher risk of stress fracture.
- Insoles can hep prevent stress fractures in the feet and legs by acting as shock absorbers. We recommend Tread Labs Ramble insoles for people who want a more flexible insole or Tread Labs Pace insoles for those who prefer firmer insoles.
What You Need To Know ---
What Causes A Stress Fracture?
Before you find yourself with a stress fracture, there may have been signs that you overlooked. Those warnings would have come from a stress reaction. That's when a bone has weakened significantly but has not yet begun to fissure. The injury becomes a stress fracture when the bone has begun to develop small cracks in the weak areas.
Both stress reactions and stress fractures are caused by repetitive actions that put force on the bone. Most occur in the weight-bearing bones of the lower extremities. Common causes of stress fractures include:
- Impact activities such as running and jumping
- Sudden increase in activity levels
- Changes in running surfaces (from dirt to cement)
- Infrequent or absent menstrual periods in women
- Foot problems like flat feet or high, rigid arches
- Bone diseases such as osteoporosis
If the risk of stress fractures in your feet and legs makes you want to stay away from impact activities like running, think again. Even though weight bearing exercises can be a cause of stress fractures, they can also help strengthen your bones.
Impact is Good For Your Bones—in Moderation
Our bones are constantly forming new cells (bone formation) at the same time that they are resorbing old ones (bone resorption). This constant state of turnover (called remodeling) allows newer bone to develop and replace old bone.
Weight-bearing exercises such as running and walking are good for the bones as they promote the development of new bone cells, and thus encourage the remodeling process.
Problems arise when your bones experience a repetitive application of force that is more than your lower extremities usually bear. Increased levels of force can cause an imbalance between the breakdown of older bone and the growth of new bone.
When breakdown outpaces growth, you will develop “bone fatigue.” Eventually, these problem areas can develop into stress reactions and stress fractures in the feet and legs.
Common Stress Fractures in the Feet and Legs
Stress fractures are most common in the weight bearing bones of the legs and feet. Some activities have a higher risk of stress fracture, including:
- Track and field
- Basketball
- Tennis
- Gymnastics
- Long-distance running
So, what are the most common types of stress fractures caused by weight bearing activities? They can be broken up into those of the foot, the lower leg, and the upper leg.
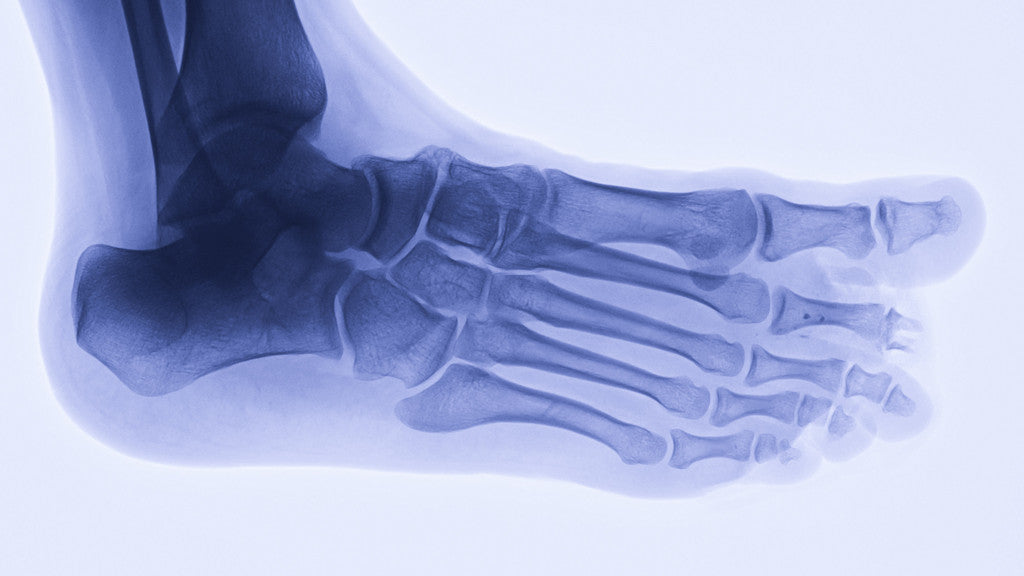
Stress Fractures in the Feet:
- Second and third metatarsals. The bones of your second and third toes are thinner than that of your first toe. The metatarsals absorb the greatest impact when you push off while running or walking. This is the most common stress fracture in the foot.
- Calcaneus (heel).
- Talus (a small bone in the ankle joint) and navicular (a bone on the top of the midfoot). These bones take longer to heal and may require a cast.
Stress Fractures in the Lower Legs:
- Tibia. This is the most common area for a stress fracture apart from the metatarsals. Initially, this will feel like a “shin splint” that doesn’t improve over time with rest.
- Fibula (the outer bone of the lower leg and ankle).
Stress Fractures in the Upper Legs:
- Femoral shaft. The femur is the large bone in your upper leg also called the thighbone. These stress fractures are common in long-distance runners and military recruits.
- Femoral neck. These are also common in runners and military recruits. A stress reaction in the neck of the femur requires complete rest and use of crutches for 6 to 8 weeks.
Stress Fractures Symptoms in the Feet and Legs
Stress fractures or stress reactions often manifest themselves as deep aches in the bone that initially get better with rest, but over time worsen, even while resting. Stretching, massage, ice, and heat do not relieve the achy feeling. There might be swelling around the injury and it could be tender to the touch.
If you are experiencing similar symptoms, you should see a doctor. It is best to see an orthopedic surgeon or sports medicine physician. Your physician should perform a thorough muscular-skeletal examination of your lower extremities. It is important they feel your muscles, test for range of motion, and perform weight-bearing tests to identify if you have a bone or soft-tissue injury.
They should also perform an x-ray. Be aware, however, that most stress fractures in the feet and legs will not show up on an x-ray. If your physician suspects you have a stress fracture after performing the muscular-skeletal exam, you will also need to get an MRI. These can detect stress reactions as early as one week in.
If you're diagnosed with a stress fracture, you should also undergo a bone-density scan, also called a DXA scan, to identify if your bone density levels are within a normal range. The scan will demonstrate if you have osteopenia (pre-osteoporosis) or even osteoporosis.
Even if you are young, it is a good idea to get a bone-density scan to understand the underlying causes of the injury. If you have strong bones, perhaps a sudden increase in training caused the stress fracture. However, if you have bone loss, you will need to begin a program of calcium and vitamin D to promote bone formation.
Recovering from Stress Fractures
When you have been diagnosed with a stress fracture, one of the most important things you can do is rest. Follow your physician’s directions. Do not try to put weight on the area until you are told to do so. It is important to let the bone heal completely.
If you get back to your normal activity level too quickly, you are at a higher risk for repeated and more serious stress fractures, and even acute breaks.
Some stress fractures require more rest and recovery than others. For example, a stress fracture in the foot may call for the use of a soft cast and crutches, but you can engage in non-weight-bearing activities like swimming and cycling.
Stress fractures in the neck of the femur often require complete rest. Recovery will include the use of crutches and no exercise whatsoever. If you don’t allow the femoral neck to heal, the fracture can eventually turn into a full-blown break, and the top of the bone will chip off from the femur, requiring surgery.
Make sure you put together a return-to-activity plan with your physician. After you allow the injury to heal, follow a week-by-week plan that begins with non-weight-bearing activities like swimming and slowly moves into walking, running, and then normal activity.
Women and Stress Fractures
Studies have found that female athletes develop stress fractures at a higher rate than their male counterparts. This is often due to what researchers have termed the “female athlete triad.” When a young woman engages in dieting or excessive exercise three interrelated consequences occur:
- Eating disorders. A lack of nutrients such as calcium and vitamin D and an overall low body weight will lead to abnormal menstruation.
- Menstrual dysfunction. Irregular or absent menstruation due to over exercise or low body weight means that your body is not producing enough estrogen, which helps your body process the calcium needed to strengthen bones.
- Premature osteoporosis. When your bone density decreases, you are vulnerable to bone injuries such as stress fractures.
As a young woman’s bone density decreases, she will have a higher risk of developing stress fractures. It is important to eat healthy, maintain a healthy weight, and exercise in moderation.
Young women who have had a history of an eating disorder and amenorrhea (the absence of menstrual periods) should make sure their food sources provide calcium as well as take calcium supplements with vitamin D to encourage bone growth.
Older women who have gone through menopause should also be aware of their increased risk of osteoporosis. Stay active and speak with your physician about maintaining a healthy diet, including supplements to support strong bones. You should aim between 1,000 and 1,500 milligrams of calcium a day.
Shoe Inserts Can Help Prevent Stress Fractures
While over-training, repetitive impact exercise, and low bone density can cause stress fractures, improper biomechanics also plays a role. Flat feet and high arches can increase the risk for stress fractures in the foot and leg.
- Flat feet can prevent the heel from acting as a shock absorber. This means the impact will transfer up the leg, and can result in tibial and fibular stress fractures. Studies have shown that arch support insoles can help prevent injuries in the tibia and fibia.
- High arches can also inhibit balanced impact absorption. Femoral and tibial stress fractures are linked to this.
- Low arches are associated with metatarsal stress fractures as the toes absorb more impact.
The best shoe inserts for stress fractures will help improve the shock-absorbing capacity of the feet and spread impact in an even manner. When shopping for insoles to prevent a stress fracture from running or other impact activities, look for:
- A deep heel cup that concentrates your heel's natural cushioning qualities and aids in shock absorption.
- Firm support that holds up under impact from the athletic activities you do.
- A precise fit in which the arch height of the insole mimics the contours of your feet.
While not everyone will develop a stress fracture, wearing proper footwear and the best shoe inserts for stress fractures will help prevent injury.
Questions? Drop us a line at hello@treadlabs.com. We're here to help.
